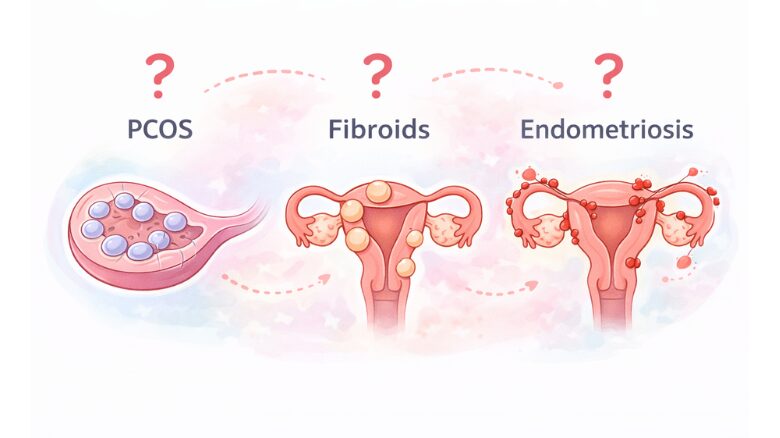
Three gynaecological conditions — polycystic ovary syndrome (PCOS), uterine fibroids, and endometriosis — collectively affect a significant proportion of women of reproductive age, yet are frequently misunderstood, under-diagnosed, or normalised as "just bad periods." At Harsha Hospitals, our gynaecology team is committed to changing that. Here is a clear, jargon-free explanation of each condition, what it means for your body, and how it can be managed.
PCOS: A Hormonal and Metabolic Condition
Polycystic ovary syndrome is one of the most common hormonal disorders in women of reproductive age, affecting roughly 1 in 10. Despite its name, PCOS does not necessarily mean you have cysts on your ovaries — the term refers to the presence of multiple small follicles that fail to mature and release eggs regularly.
The core issue is hormonal imbalance: elevated androgens (male hormones) and insulin resistance disrupt ovulation and create a cascade of symptoms including irregular or absent periods, acne, excess facial or body hair (hirsutism), difficulty losing weight, and fertility challenges. PCOS also increases the long-term risk of type 2 diabetes and cardiovascular disease if left unmanaged. Treatment is tailored to each woman's priority — whether that is regulating periods, managing acne, improving fertility, or reducing metabolic risk — and typically involves a combination of lifestyle changes, hormonal therapy, and medication.
Fibroids: Non-Cancerous Growths With Real Symptoms
Uterine fibroids are benign (non-cancerous) muscular growths that develop within or on the wall of the uterus. They are extraordinarily common — many women have them without ever knowing it. However, fibroids that grow large or in certain positions can cause heavy and prolonged periods, pelvic pressure or pain, frequent urination from pressing on the bladder, and difficulties with fertility or pregnancy. Fibroids are oestrogen-sensitive, which means they tend to grow during the reproductive years and shrink after menopause. Treatment options range from medication to manage symptoms, to minimally invasive procedures such as uterine fibroid embolisation, to surgical removal (myomectomy) depending on size, location, and the woman's reproductive plans.
Endometriosis: When Tissue Grows Where It Should Not
Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus — on the ovaries, fallopian tubes, bowel, or bladder. Each month, this tissue responds to hormonal signals and attempts to shed, but with no pathway out of the body. The result is inflammation, internal bleeding, scar tissue (adhesions), and intense pain — particularly during periods, intercourse, bowel movements, or urination. Endometriosis is notoriously under-diagnosed, with an average delay of 7 to 10 years from symptom onset to confirmed diagnosis.
It is a leading cause of infertility and chronic pelvic pain. Treatment includes hormonal therapy to suppress the cycle, pain management strategies, and laparoscopic surgery to remove endometrial deposits. There is currently no cure, but with expert management, most women achieve significant symptom relief.
 Key Message from Harsha Hospitals: None of these conditions are simply "part of being a woman." Painful periods, irregular cycles, and unexplained weight gain are symptoms, not character traits. If you recognise yourself in any of these descriptions, a specialist consultation is the most important step you can take for your long-term health.
Key Message from Harsha Hospitals: None of these conditions are simply "part of being a woman." Painful periods, irregular cycles, and unexplained weight gain are symptoms, not character traits. If you recognise yourself in any of these descriptions, a specialist consultation is the most important step you can take for your long-term health.


